Preventing, Treating & Living With Osteoporosis

Dr. Christina Jones
As the U.S. population ages, certain diseases and medical conditions more common among aging Americans are gaining greater public attention. Osteoporosis, a serious, disabling disease and the most prevalent metabolic bone disease in Western societies is one such condition.
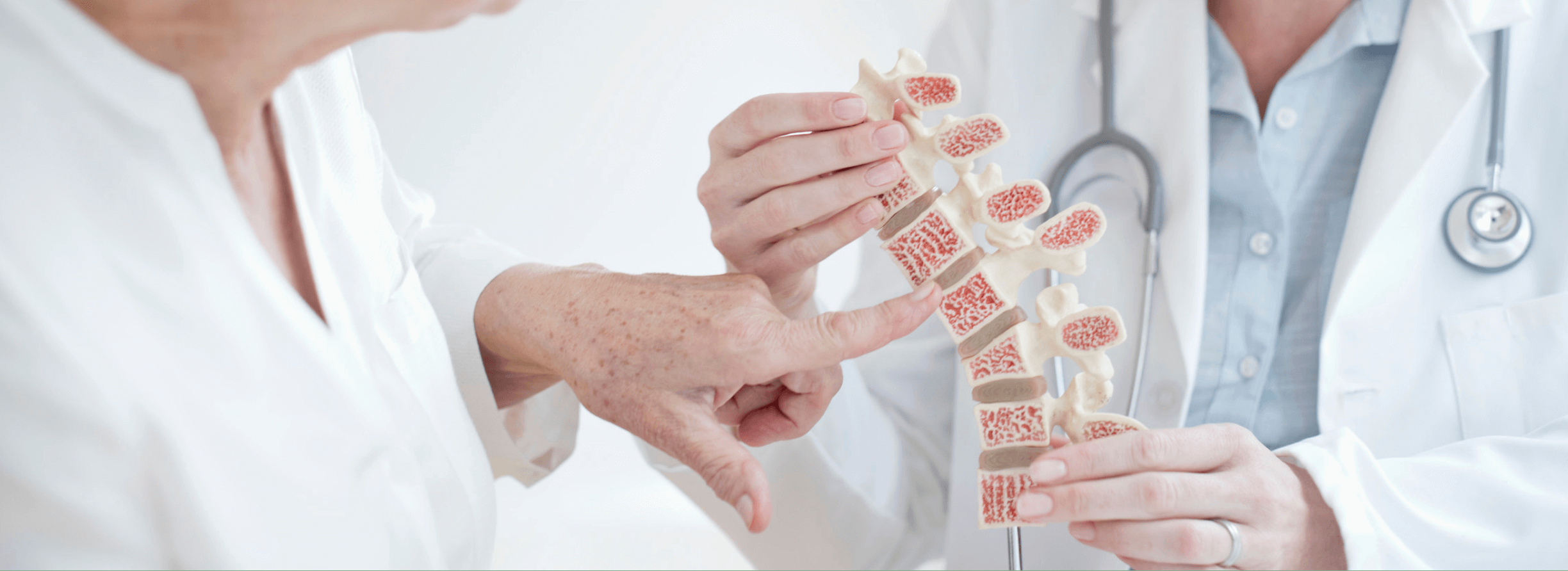
Fortunately, osteoporosis can and should be prevented and, when present, treated. In the United States alone, it affects 25 million people and causes 1.5 million fractures annually.
Risk Factors for Osteoporosis
Osteoporosis is defined as a skeletal disease characterized by low bone mass and deterioration in bone microarchitecture leading to bone fragility and susceptibility to fracture. The World Health Organization (WHO) has defined osteoporosis as a bone mineral density that is 2.5 standard deviations (SD) below the mean peak value in young adults. This is called the T-score. A T-score that is between 1 and 2.5 SD below the mean is called osteopenia.
Race
Most cases of osteoporosis occur in postmenopausal women and the rate increases with declining BMD (bone mineral density) and with age. In the United States, the rates of osteoporosis and fractures vary with ethnicity, with African Americans having the highest BMD and Asian-Americans having the lowest. Of white American women, 13 to 18 % who are 50 years or older have osteoporosis of the hip. An additional 37 to 50 percent have low bone mass (osteopenia) of the hip again increasing with age.
Menopause
As we age, bone resorption increases. This increase is worsened by a decrease in bone formation in women after menopause. Within the first few years of menopause, there is rapid bone loss due to lower levels of estrogen production. The decline in estrogen is the most significant factor in the increased bone loss associated with menopause.
Age
Genetic predisposition also contributes significantly to bone mass and to the development of osteoporosis later in life. Hereditary has the greatest influence on a woman’s peak bone mass, and studies have suggested that 80 percent of the determinant of peak bone density is due to genetic factors.
Diet
Dietary factors and nutrient deficiencies alter bone growth and remodeling and may result in lower bone mass. People with a dietary abnormality such as anorexia nervosa have significantly lower bone mass than their healthy counterparts. A balanced diet of plenty of vegetables – especially dark green leafy vegetables – nuts, seeds, and whole grains, along with adequate calcium and vitamin D intake is needed to achieve a peak bone mass.
How Do I Know If I Have Osteoporosis?
The evaluation of risk and diagnosis of osteoporosis is made by a careful medical history, a thorough physical examination, laboratory analysis, and measuring bone density. The most common risk factors for osteoporotic fractures are female, advanced age, low BMD, and previous fractures as an adult. It might be tempting to think that all menopausal women should have a bone density test. However, the recommendations for BMD testing – DEXA scan- from the North American Menopause Society states that should be: postmenopausal women with medical causes of bone loss, all postmenopausal women who are 65 years or older, postmenopausal women younger than age 65 who have one or more of the following risk factors for fracture such as fracture after menopause, weight less than 127 pounds or BMI less than 21, hip fracture in their mother or father and/or current smoker.
How Can I Prevent It?
Osteoporosis is far easier to prevent than to treat. An osteoporosis prevention plan needs to start in the teenage years. For women in their 40s, 50s, and older who are just beginning to think about osteoporosis, the time for reaching peak bone density at age 30 to 35 has already passed. Several approaches are available to prevent osteoporosis. These include not smoking, reducing or avoiding alcohol, doing regular weight-bearing exercise (especially comprehensive weight lifting) throughout life, ensuring proper nutrition, avoiding being underweight, minimizing caffeine intake, reducing animal protein, considering hormone replacement therapy (either bio-identical hormones or conventional if with several risk factors), and taking nutritional supplements for bone health.
Osteoporosis is one of the most important age-associated disorders and should be considered a potentially disabling disease that warrants substantial preventive efforts and management interventions. Early identification of risk factors for osteoporosis, prevention strategies, vitamin D status, and assessment of calcium metabolism and bone density provide the basis for the determination of what is appropriate for each person. Your family physician, internist, endocrinologist, and/or gynecologist are probably the cornerstone for medical therapy and detection.
Hopefully, we’ve been able to teach you a little something about this common, yet preventable, condition. If you are currently concerned that you may have this condition or another related disorder, then it’s important to speak with a doctor as soon as possible.
Request a Free Demo
Learn how Radish Health can help you improve employee health and save on healthcare.
Request a Demo